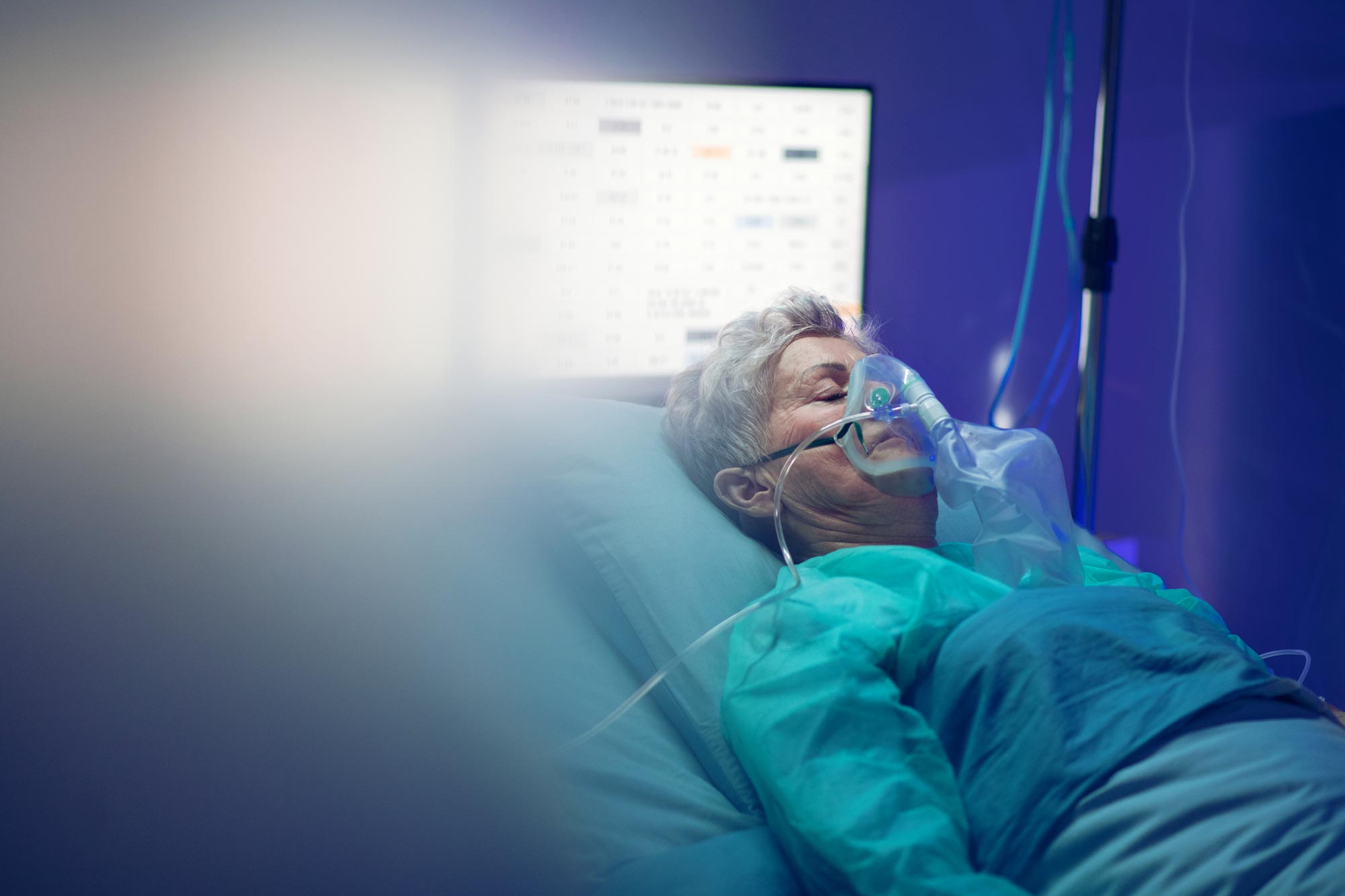
As COVID-19 cases spike across the United States and intensive care units reach near-capacity, physicians at UVA Health are working to manage caseloads and provide optimum care to COVID-19 patients.
Dr. Catherine Bonham, an intensive care physician on UVA Health’s COVID-19 ward, studies how the human immune system responds to viral infections. Using a new rapid response grant from the University of Virginia’s Office of the Vice President for Research, she and pulmonary care colleagues Dr. Alexandra Kadl and Dr. Lindsay Somerville are examining the immune responses of COVID-19 patients, and how it differs from influenza infection.
Here, Bonham discusses COVID-19 for readers of UVA Today.
Q. What challenges are you facing on the ICU?
A. Every winter we prepare for patients with respiratory failure from the flu. Some years are worse than others, and this past flu season was particularly bad. Then the pandemic came and we had to open an entirely new ICU and acute care unit to care for COVID-19 patients. The present test to the health care system is responding to our usual demands, and flexing up to the challenges presented by this new infectious disease.
The care we provide to COVID-19 patients comes from a foundation of knowledge that is very familiar to us in treating patients with acute respiratory failure from the flu. A lot of what we know, in terms of how to treat low oxygen levels in the lungs, has been rigorously tested and proven during many years of treating people with the flu. Fortunately, at UVA we have the resources and experience to do this well.

Dr. Catherine Bonham is a pulmonary care physician on UVA Health’s COVID-19 ward and a researcher studying pulmonary fibrosis and immune responses. (Photo courtesy UVA Health)
COVID-19 presents new challenges; new nuances. For example, these patients have a high tendency to form blood clots. This has resulted in new protocols for giving anti-coagulation medications.
Most of our COVID-19 patients in the ICU need to be on a ventilator for a lengthy period of time – about two weeks on average. This is not always the case in people who have the flu. Being on a ventilator for a long time results in complications, including the need for sedation medications to help the patient tolerate the breathing tube. One of our key challenges is to make sure the patient is properly oxygenated while minimizing the delirium and confusion that sedation can cause.
Q. How many COVID-19 patients are you treating?
A. It varies. We have had anywhere from six to 17 patients in the ICU at any time, and dozens more who don’t meet ICU needs but are on the hospital wards receiving oxygen and other therapies. We are caring for patients from within the community as well as from hard-hit counties outside of our area.
We have been really fortunate in that we have not been overwhelmed. And we have worked hard to ensure that we have the resources and staff to appropriately care for our patients.
Q. How does COVID-19 compare with the flu?
A. Death rates are higher from COVID-19 than the flu. The situation is evolving, and we won’t know the long-term outcome – the patient recovery rate from COVID-19 – until months from now. It may be that the number of people who need treatment are the tip of the iceberg in terms of total infections. I am almost certain that as we do more testing and get a better grasp on how many people have been infected, the mortality rate will go down. But that could be said of the flu as well, if we tested extensively for it.
This novel coronavirus appears to be not only highly contagious, but it also sickens a high number of people, requiring hospitalization. Even during a bad flu year, we don’t see anywhere near the number of patients coming in that we’ve seen with COVID-19. A once-in-a-lifetime infectious event like this can overwhelm hospitals. It can make mortality rates look worse because our health care system generally does not have the capacity to care for large numbers of patients getting sick all at once.
This is why social distancing is so important – it reduces the number of people getting sick all at once, putting less strain on our health care system.
Q. Are you seeing younger patients with COVID-19?
A. Yes, we have had young people come in who were extremely ill, needing ICU care and ventilation. We’ve seen a fairly representative slice of age ranges, including individuals who previously had only mild health problems, and some who had no other health problems, and, yet for some reason, they’ve been severely affected by this virus. This is why our research is so important to understanding what, at the cellular and molecular level, is driving so many critically ill outcomes.

We’re testing a couple of hypotheses. One is that a subset of patients has a very high inflammatory response to this virus, and this inflammatory response results in high levels of pulmonary edema, which is fluid in the lungs. This can also cause blood clotting, and ultimately the need for ventilation.
We also see critically ill patients with extremely low white blood cell counts. Their adaptive response, which makes antibodies, has been handicapped in some way. A number of patients also get bacterial infections. This makes me think that their adaptive immune response has either been exhausted or become dysfunctional in the face of COVID-19 infection, and we’re working to better understand this.
We’re finding that critically ill patients can have significant problems with weakness and delirium after they leave the hospital. Survivorship after critical illness can take months.
One of my great hopes, as an outcome of the pandemic, is that we become better at supporting people who have survived critical illness of any type. We need advocacy for critically ill survivors. We are learning important things – not only how the immune system responds to a virus – but how to effectively rehab patients after a long illness so they can again be functional.
Q. How are you treating patients with COVID-19?
A. We are using proven therapies. We know that the antiviral medication remdesivir will help and not harm patients, and the steroid dexamethasone helps with inflammation, so our patients are receiving those drugs when appropriate. We also are conducting clinical trials for some promising therapies.
With application of evidence-based supportive care, we can treat COVID-19 as effectively as any viral pneumonia. This includes adjusting ventilators so as not to cause injury to the lungs, optimally positioning our patients so they can best receive oxygen, smart management of intravenous fluids to avoid complications like kidney failure, and, very importantly, using a team approach to treatment where physicians, nurses and technicians employ best strategies for each patient’s care.
Q. What are your concerns as we navigate this pandemic?
A. I’m concerned as we are seeing spikes in critical cases, and I’m not sure we as a nation have the safety net needed for critical care survivors, particularly people who are uninsured or underinsured.
I’m also concerned for patients who develop pulmonary fibrosis, which is scarring of the lungs. That leads to significant disabilities requiring long-term oxygen.
But as we continue to learn, we are getting better at treating COVID-19. I’m cautiously optimistic that we will eventually have a vaccine and effective specific treatments for this disease.
Q. As more people become infected, will we develop herd immunity?
A. To develop herd immunity, about 80% of the population must become infected and immune. It’s a long and dangerous road; as many people will get severely sick and die along the way.
The challenge will be finding vaccines that give long-lasting, durable immunity. In non-novel coronavirus, immunity can last two to three years at best. With the novel coronavirus, studies indicate that immunity may start declining within several months. We will need to innovate a vaccine that provides long-lasting immunity.
Q. Do you think we can safely get back to work and school?
A. We can’t keep the economy closed forever. We’ve seen in Europe and other parts of the world that cautious reopening can occur safely. I think it’s very possible here, too, but we need a concerted effort by our fellow Americans and government leadership to demonstrate that public health measures like masking, hand-washing and reducing time in large gatherings can allow us to open and minimize infections. I think we will get there, but, in the meantime, we are experiencing learning curves in balancing economic viability and public health policy.
Infection depends on close proximity – the length of time spent with an infected person, how much virus is shed, and if contact is sustained in an enclosed space, such as a bar.
There is little evidence that people are getting infections from minimal interactions, like picking up some groceries. So wear a mask, don’t touch your face or rub your eyes, wash or sanitize your hands after a trip out.
Q. Does a mask provide any personal protection, or is it strictly protective for the people around you?
A. Surgical or cloth masks block large-particle droplets, respiratory secretions and saliva. They are helpful to the wearer for this blocking effect and to remind you not to touch your nose and mouth.
Masks are especially helpful to the people around you. If I’m wearing a mask, I’m keeping you safe. If you wear a mask, then you are keeping me safe, too. This is something we should do for each other.
We’re learning a lot, together, and eventually we will come out of this better, together.
Media Contact
Article Information
July 14, 2020
/content/qa-front-lines-dr-catherine-bonham-talks-covid-19