Who would choose to get sick?
Well, second-year University of Virginia student Jonathon Rimmington, among others.

On his 20th birthday, Rimmington dutifully reported to the Infectious Disease Study Center to be politely infected with rhinovirus, the most ubiquitous cause of the common cold.
For a few days of sniffling and sneezing – and periodic check-ins over the next several months – Rimmington and several others will each be paid $1,200 for their trouble.
The volunteers are taking part in the cold study, a UVA institution that has subsidized many a tuition since its inception in the 1970s. Over the years, the study has shed much light on the common cold, illustrating the ways in which the virus can spread – and the difficulty of treating it.
“The idea is to take human volunteers – and in the case of UVA, it tends to be students – and assess them to see whether they’re susceptible to our rhinovirus. And then we intentionally infect them with the rhinovirus and we can monitor what happens to them after they’re infected,” explained Dr. Ronald B. Turner, a professor of pediatrics who leads the study.
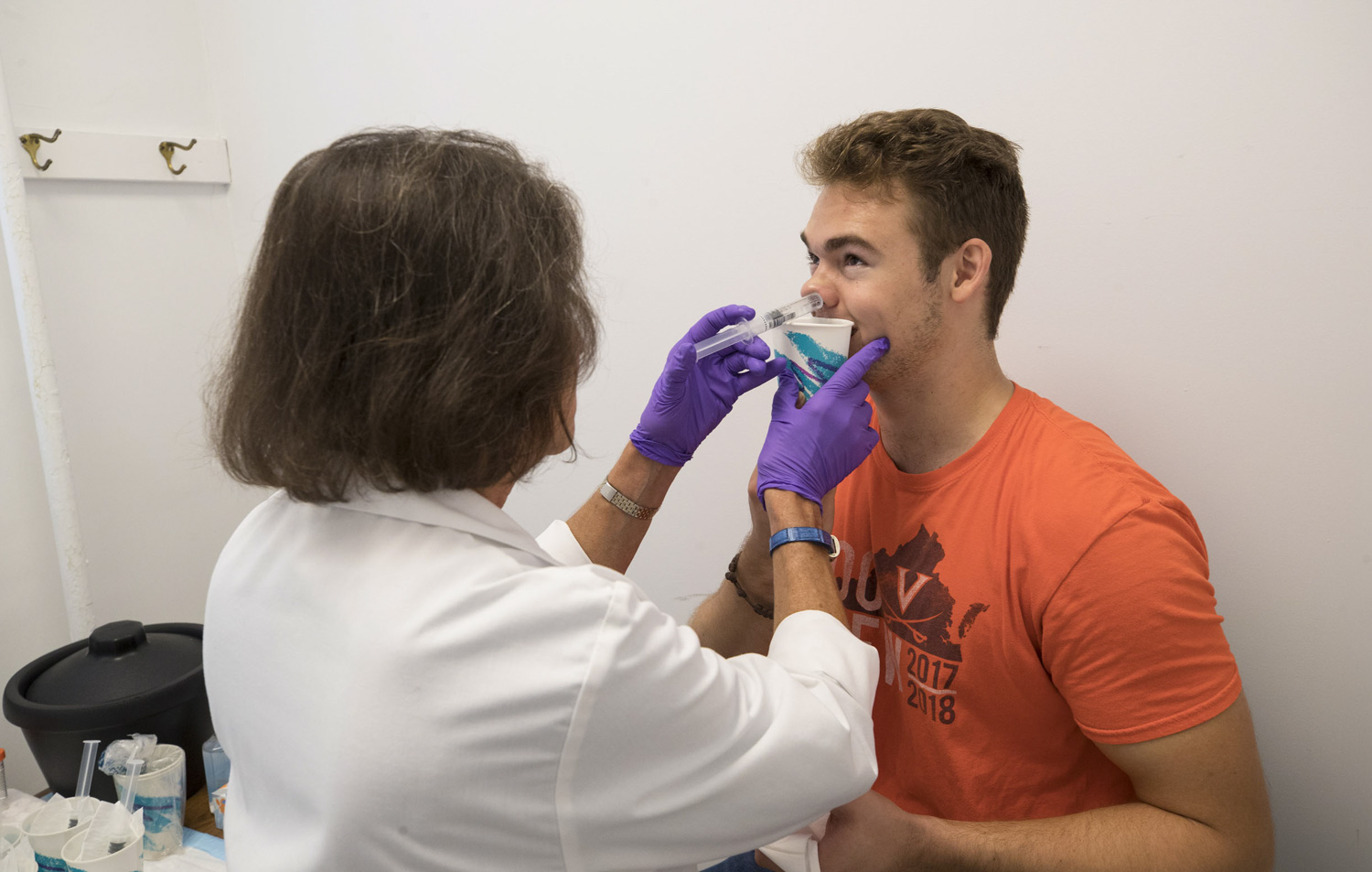
For $1,200, second-year student Jonathon Rimmington will be infected twice with rhinovirus, a cause of the common cold, and check in periodically so researchers can study his immune response. (Photos by Dan Addison, University Communications)
The model is unique, with no one else in the U.S. currently conducting rhinovirus challenge studies.
The study Rimmington is participating in is funded by the National Institutes of Health and will focus on the immune response to the virus. The volunteers who were recently infected will check in through January, at which point they will be infected again, some with a different serotype of the virus.
“These are fairly mild illnesses and most people’s symptoms are essentially gone after week one,” Turner said.
Emma Thurman, a third-year student who volunteered, said the inconvenience was “definitely” worth it. Thurman said she doesn’t often get sick and would be using the extra cash for graduate school.
“I’ve got three sisters, so my dad has given us the hard cut-off at undergrad,” she said. “So we need money.”
Rimmington decided to volunteer with a friend after seeing the study advertised on Grounds. He said it was all about the cash, noting that a check coming in around Christmastime would be nice.
As an afterthought, he added, “and for the sake of science, I guess, if I’m talking to someone I want to impress.”
Coming Into the Colds
Turner did his training here in the late 1970s with Dr. Jack Gwaltney and Dr. Owen Hendley, who were the first at UVA to conduct the rhinovirus human challenge studies, in which a healthy volunteer is infected to study the virus and its treatments.
“We became one of the important centers in the world for doing cold research,” Gwaltney said.
Gwaltney began work on the common cold in the 1960s with Dr. William Jordan, including a study done in conjunction with a State Farm Insurance Company office, then located near Barracks Road in what is now UVA’s Carruthers Hall. Gwaltney and Jordan kept a continuous record of any colds the employees had and looked for any patterns in how the virus spread.
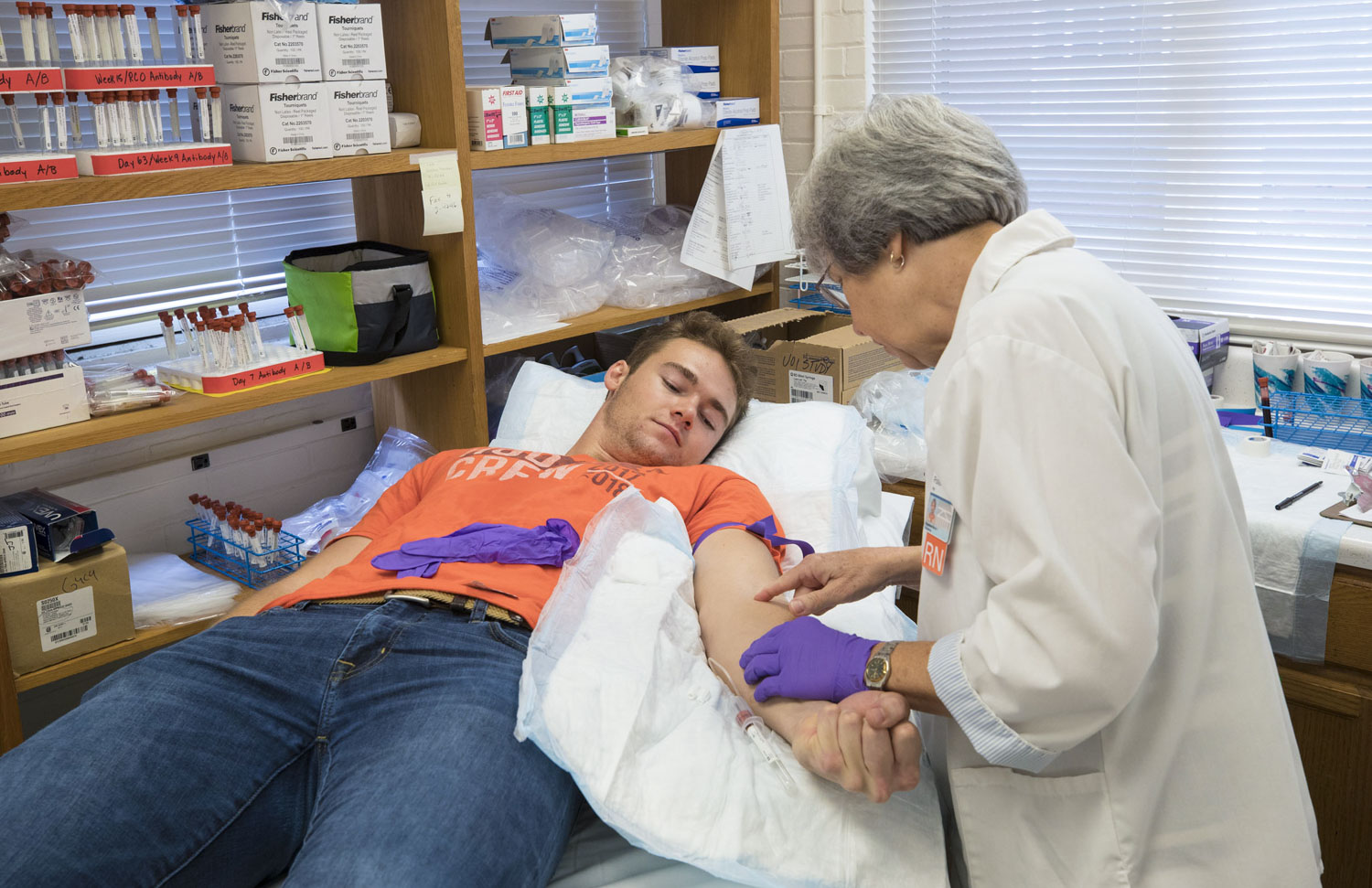
Rimmington said he agreed to be studied for the money, which would come in handy around Christmas, “and for the sake of science, I guess.”
After noticing that the virus did not seem to be spreading at work, they expanded their study to the families, discovering that in most cases it was children who became sick first, often in September.
They also conducted tests on how the virus spread, by direct contact and hand contamination, having volunteers live together for three days in area motel rooms.
“They actually contributed a significant amount to our understanding about how viral transmission occurs from one individual to another. That was a big advance,” Turner said.
“The other thing that we did that I think was quite useful was we were able to show that the reason that you get sick when you get the virus was not any direct effect of the virus,” Turner added. “Rather, it’s the host response to the virus that makes you sick. It’s the immune response. That’s one of the reasons why it’s so difficult to find a treatment for these infections.”
Though no foolproof cure for the common cold has yet been discovered, Gwaltney did find something close in the form of interferon and a three-component treatment that would block the virus from growing, but include anti-inflammatory substances and an antihistamine.
While the treatment was effective, it ended up being cost-prohibitive in the end to develop a commercial product.
“It does work. And there really is nothing that has come on since then that has better promise as far as I know,” Gwaltney said.
Making Inroads
Turner came back to UVA in 2001 and soon took over where his former mentor Gwaltney, who retired in 2004, left off.
Much of what the cold study has accomplished in recent years has been continuing to show that there is no simple cure for the common cold.
“I think that in some ways, one of our successes has been that we’ve been able to, in a very objective and controlled way, show that some things like echinacea don’t work,” Turner said.
That was also the case in a recent study, funded by Dupont, of probiotics, looking at whether they had an impact on the host’s response to the virus.
“There was a little bit of evidence – which it turns out probably is not true – that probiotics may be useful for common cold prevention,” Turner said. “The question was: does the probiotic modify the way your body responds to the virus?”

The answer to that appeared to be no. But the study led to an unexpected finding that Turner counts among the highlights of his cold research. Turner and others eventually determined that the mix of organisms that live inside your nose correlates with the type and severity of cold symptoms you develop.
“The probiotic didn’t really have any effect on your microbiome, but your microbiome was associated with differences in how you responded to the virus and whether or not you got symptoms,” Turner said.
“Because we have a longitudinal study where we can follow these volunteers over several weeks and know exactly when they got infected, we have the advantage of being able to say, ‘Hey, the microbiome was there before the virus,’” he added. “It’s a nice illustration of the utility of the model.”
An Uncertain Future
With Turner due to retire in 2021, the future of the cold study at UVA is uncertain.
“I really don’t know what’s going to happen,” Turner said, noting that the work is specialized, and costly.
A group at Duke University has expressed interest in taking over the two strains of the virus Turner has had approved by the FDA for use in human volunteers, though there has also been interest from a team at UVA immunology that has been using the rhinovirus challenge model in asthma studies.
“I have thought about giving my pools to Duke,” Turner said, “but if our folks here want it and can manage it, that would be preferable.”
Gwaltney said he would be sad to see the cold study cease to exist at UVA, but understands the difficulty in keeping the work alive.
“When I started, cold research was a very trendy, popular thing – a lot of interest in trying to find a cure for the common cold. And there was a lot of government support for it,” he said.
Now, with the government out of cold treatment and very little political support for cold treatment with health care costs already soaring, the end of an era seems near.
“These activities are so fragile and so hard to build up and it’s so easy for them to collapse if they don’t have support,” Gwaltney said. “Turner is the last Mohican we’ve got.”
Media Contact
Article Information
October 24, 2018
/content/uvas-four-decade-quest-cure-common-cold-nearing-end

